Mobile App
Motive
Improving the at home physical therapy experience.
Role
Research
UX Design
Prototyping
Videography
Problem
Patient adherence is widely problematic in the medical field and physical therapy is no exception. Failure to complete exercises as prescribed slows a patient's recovery, wastes money and causes lasting health consequences. With the help of Premera Blue Cross, this project addressed:
How can I motivate adult physical therapy patients with acute, orthopedic injuries to adhere to their home exercise programs?
Research
Secondary Research
To better frame our project, I began with secondary research in the form of an academic literature review and a competitive analysis. I learned that current tools for physical therapy adherence are not working because they:
- Try to replace the role of the physical therapist.
- Are not personalized to a patient’s specific needs.
- Do not accurately represent the patient’s exercises.
Primary Research
The primary research was framed by my secondary research and offered rich, first hand accounts of stories and experiences. My team and I employed the following techniques:
Empathy Building
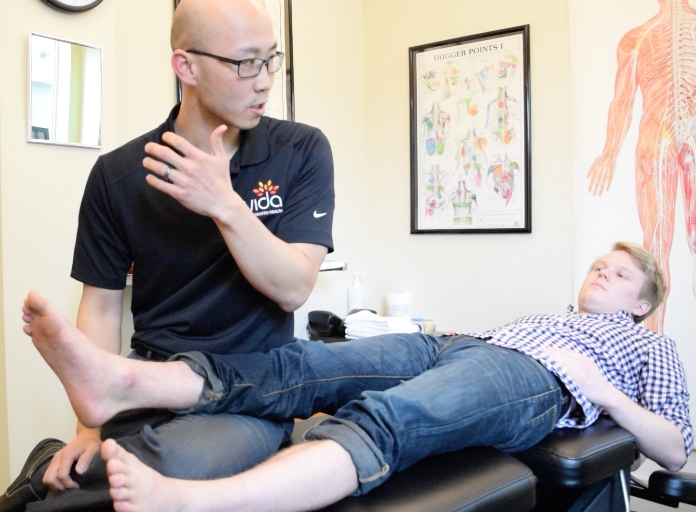
I began with an empathy building activity to familiarize ourselves with the process. A licensed physical therapist walked me through a typical first appointment and assigned us exercises to practice.
Contextual Inquiry
By conducting interviews in people’s homes, I observed environmental factors that may have affected their adherence such as what it's like to complete exercises while being walked on by a cat and a toddler.
Patient Interviews
After hearing from healthcare providers, we interviewed 6 patients ranging in self-identified adherence levels, and stages of treatment.
Expert Interviews
To help the team scope the problem space, we interviewed 6 physical therapists with a diverse set of specializations.
Research Synthesis
At several points along the way, the team discussed our findings and used affinity mapping, interview coding, concept diagrams and discussion to evaluate our results. Below are journey maps and design principles.
Experience Maps
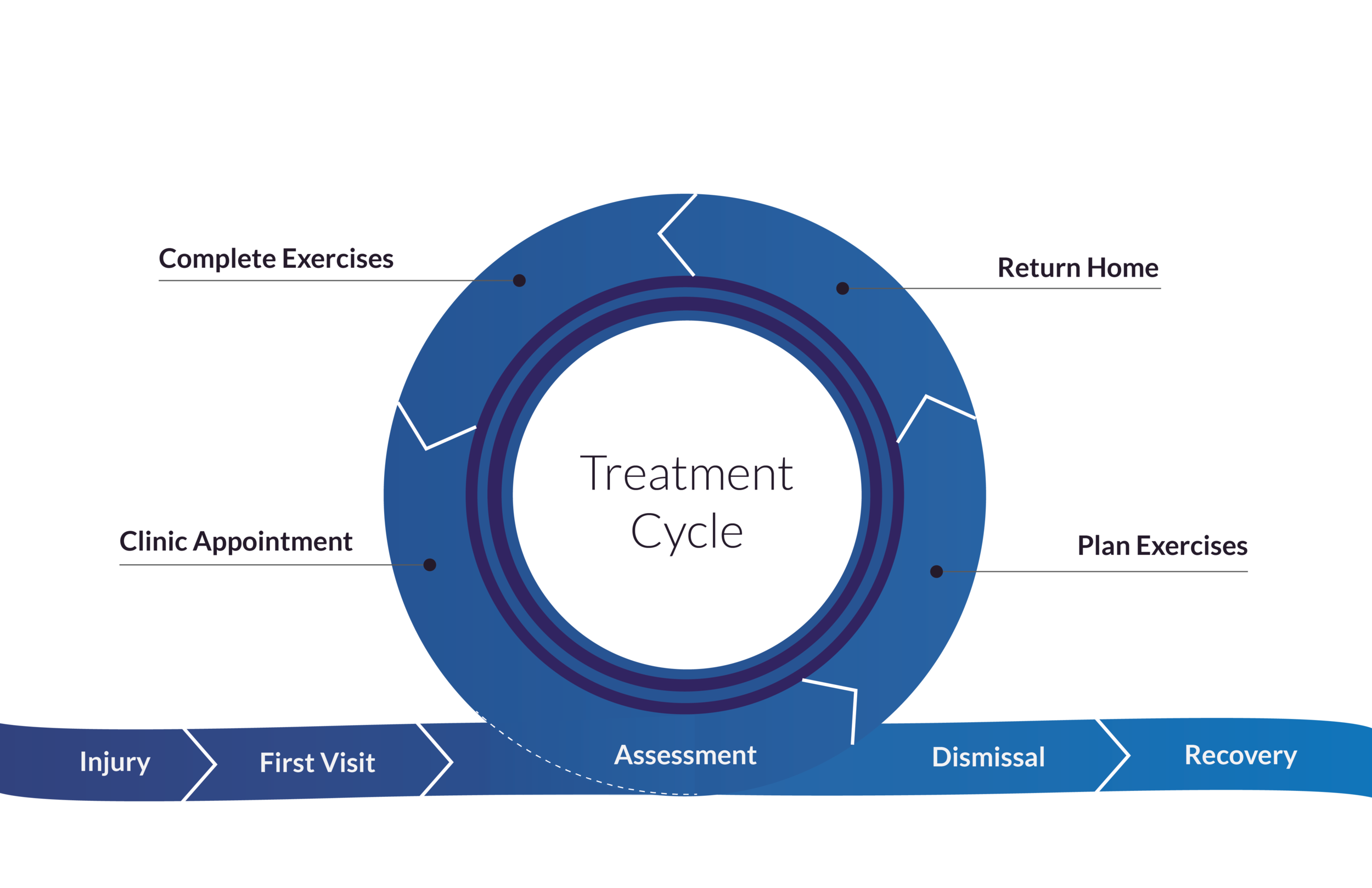
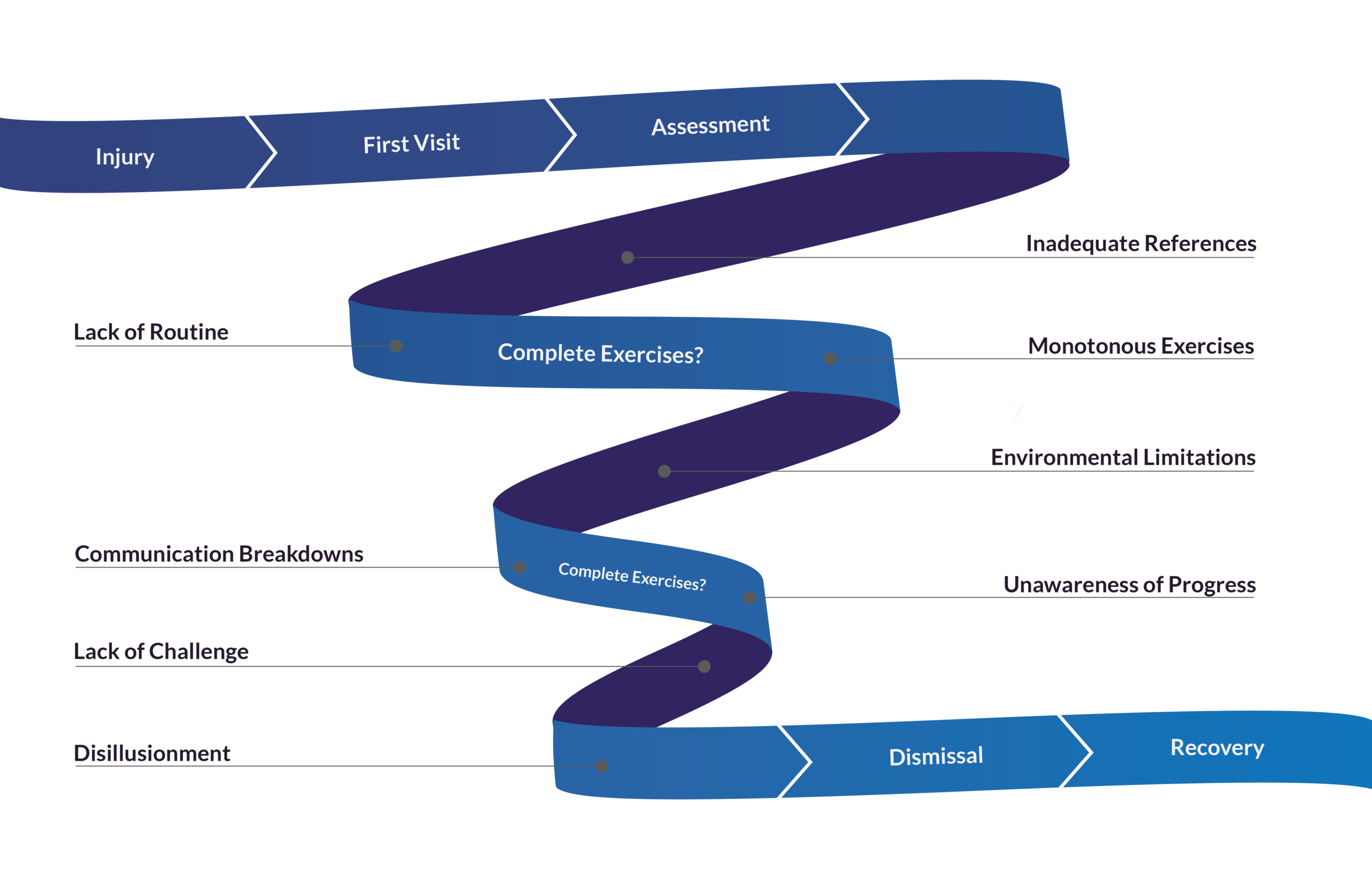
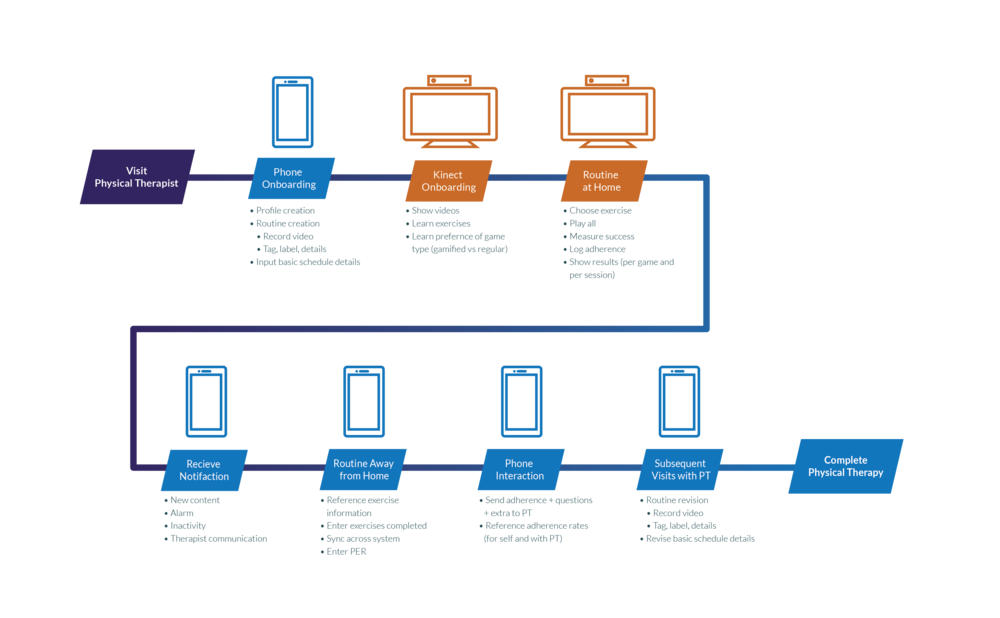
Prior to our primary research, I was under the impression that the patient experience looked like the first diagram. The patient would visit a physical therapy clinic, be expected to complete their exercises at home, and return for assessments until they were healthy enough to stop.
However if we pull apart the treatment phase, we see instead of being a consistent loop, little breakdowns along the way start to compromise a patient’s path to recovery. My research showed that patients did not feel confident remembering their exercises, were unaware of their progress, grew bored, and struggled to communicate their concerns during appointments.
Ideation
Overview
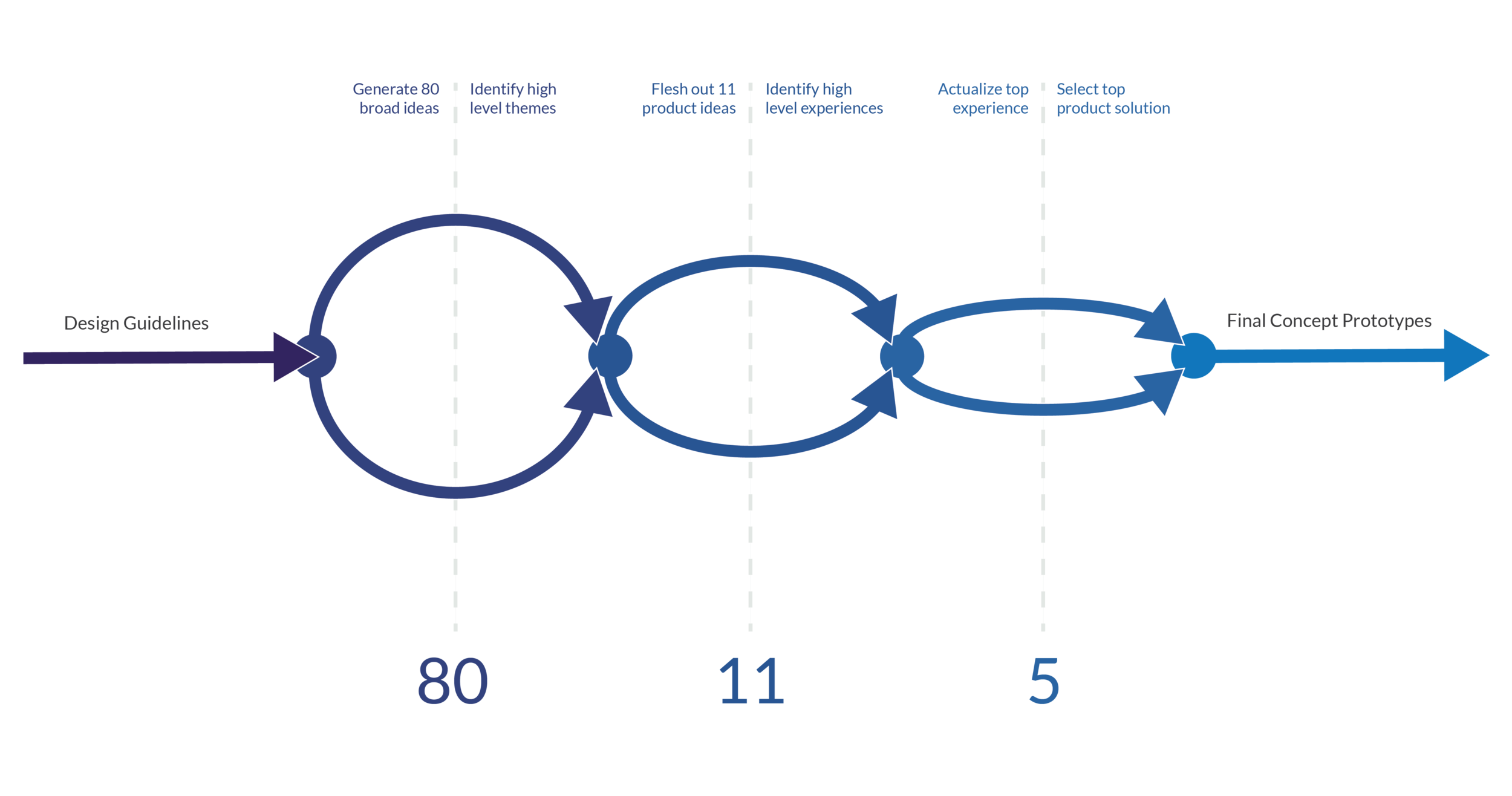
The ideation process followed three phases of individual expansion and group contraction phases.
Sketches and Storyboards
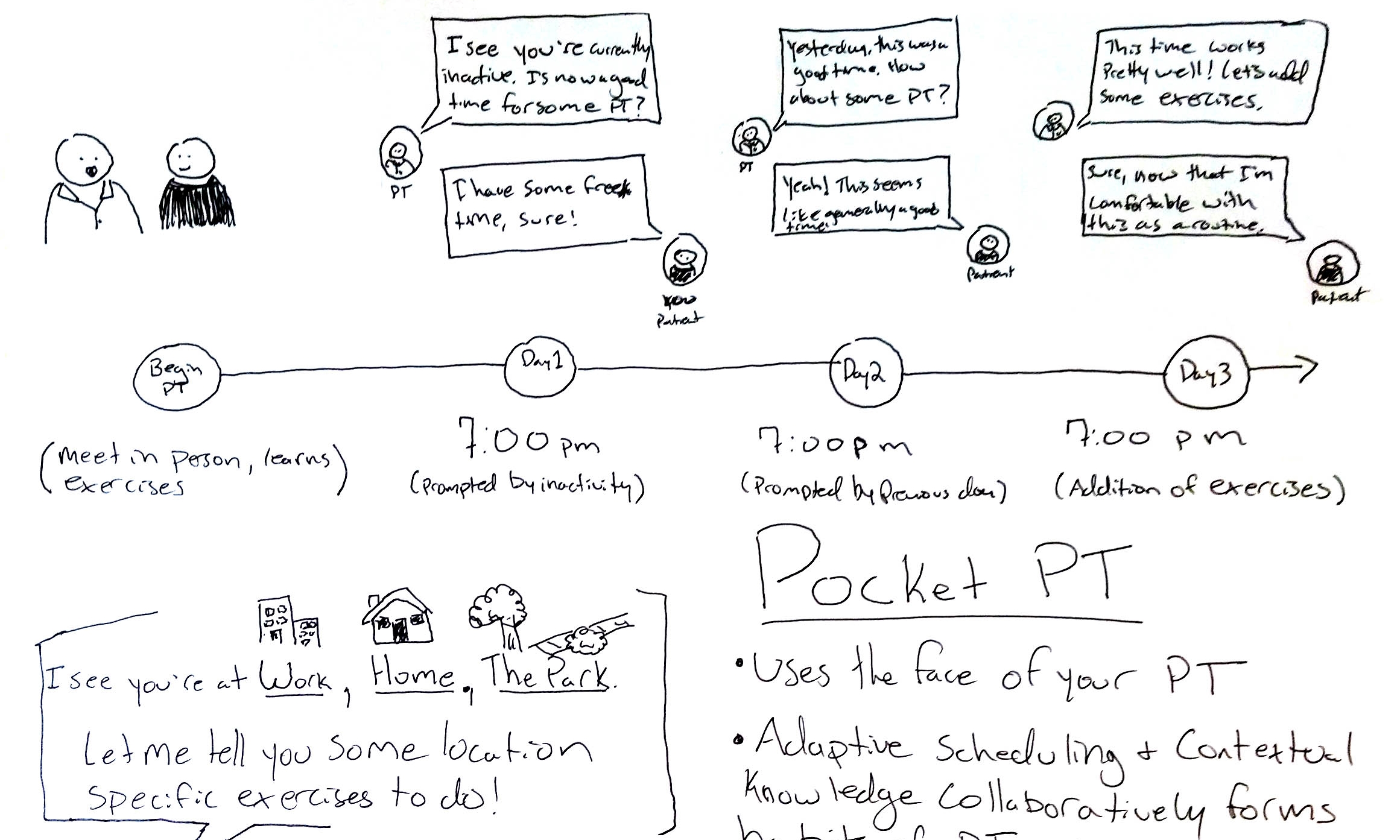
The team and I began with individual sketching with broad ideas created from a set of ideation prompts, drawn from the user research. Through the multiple week process of storyboarding and imagining what each final product might look like, I was able to discard and collapse features and interactions into our final direction.
First round thumbnail sketching
Solution based approach
Final Direction
In our ideation process, I created a list of values that reflected qualities the solution should have. I vetted solutions we had against these values and arrived at our final product, Motive.
Prototyping
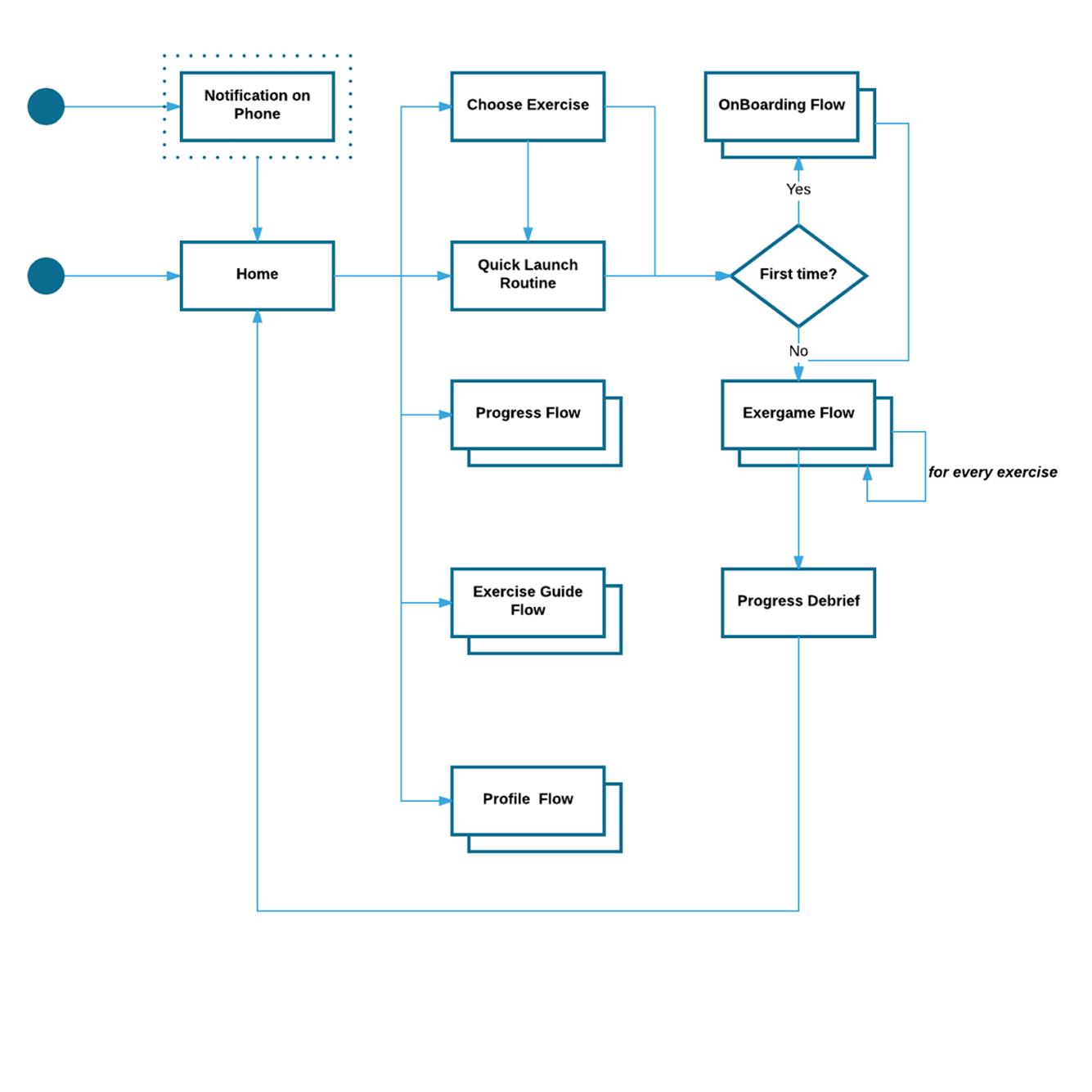
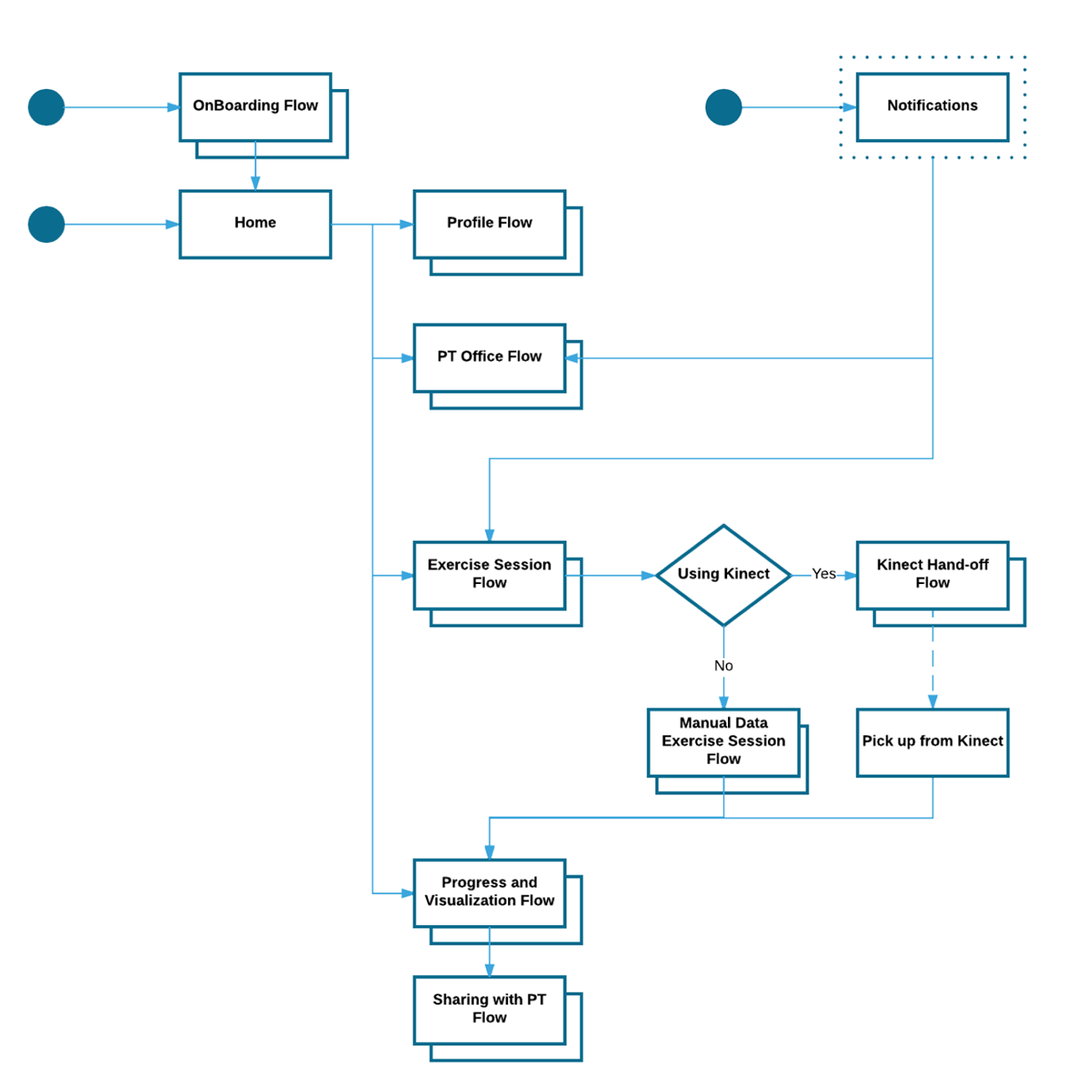
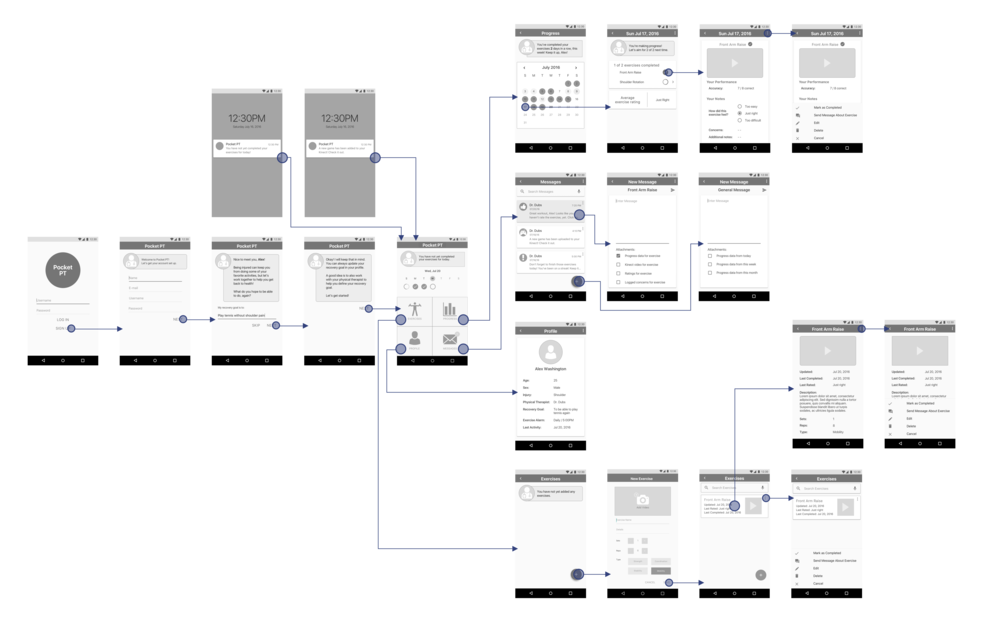
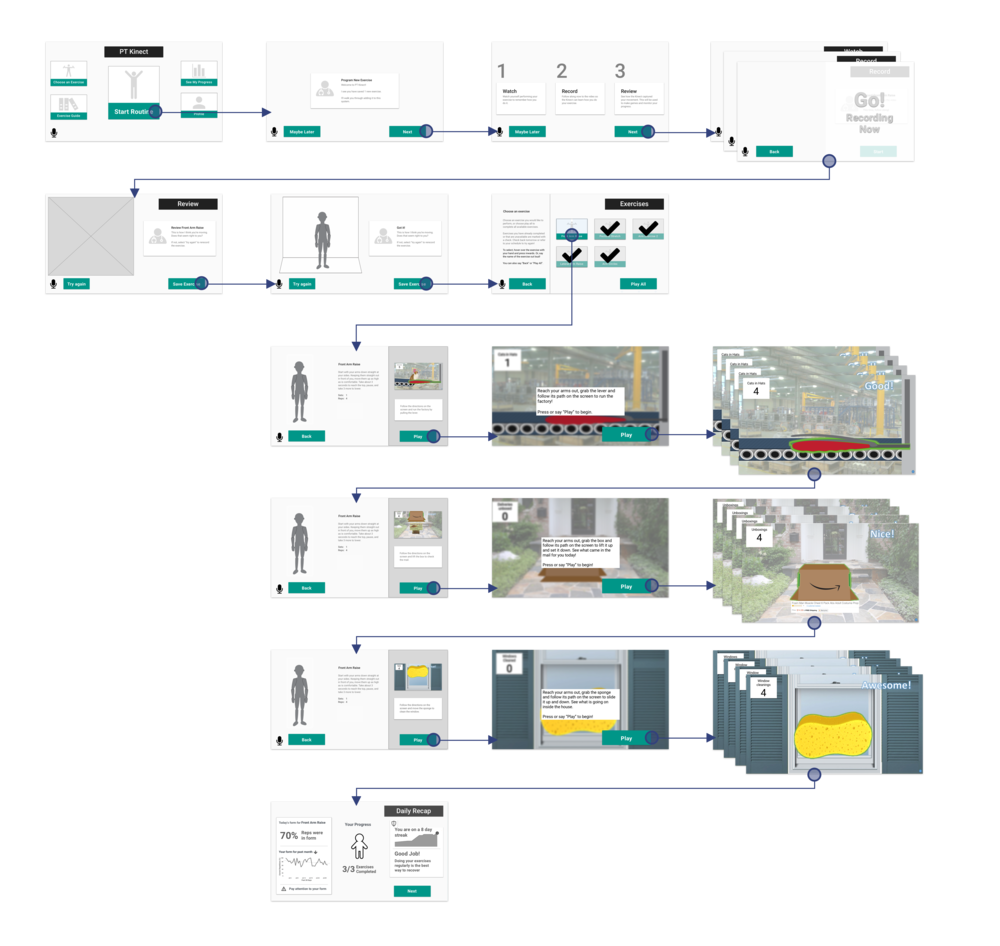
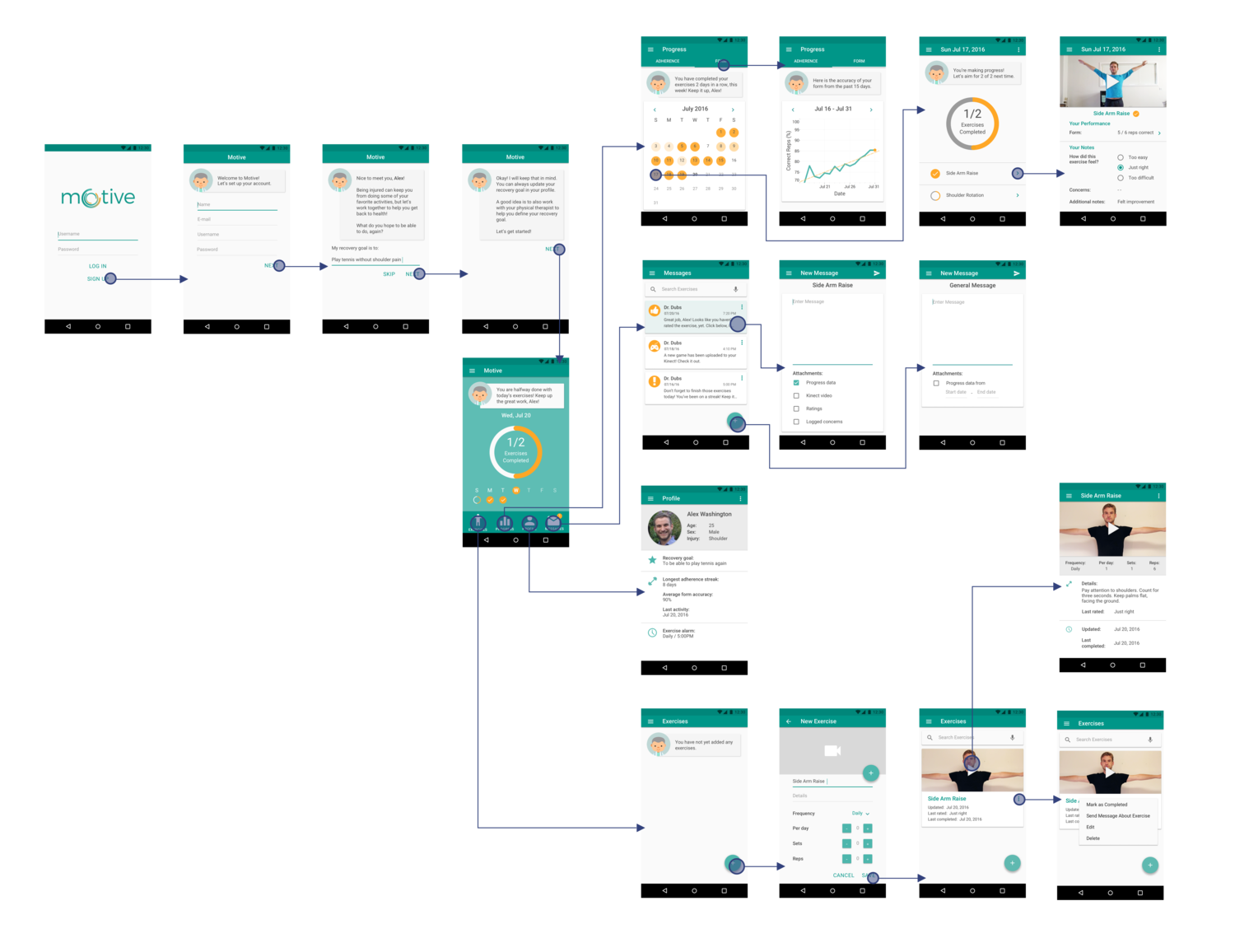
To test these ideas, we built prototypes of the Motive system. First though, I used user flow diagrams to select what paths were most pertinent to testing. Next, the team and I created mockups and a research protocol to run participants through.
Prototyping
To improve and validate these ideas, I recruited former physical therapy patients for testing after running a pilot test.
total of four participants tested the prototypes in either a private room set up in a campus library, or in the living room of their home. Participants ranged in gender, age, self-identified adherence rates, injury type, and current status of treatment. Testing through a scenario based, semi-structured interview allowed us to have participants interact directly with our prototypes in an imagined context (i.e. at the clinic, in their living room). They responded with quantitative scales and qualitative evaluations.Hypotheses
My hypotheses were the following:
- Narrated video references will increase a patient’s confidence when completing exercises at home.
- Gamified exercise experiences will keep patients more adherent than unprompted physical therapy.
- Explicit progress tracking will motivate patients to adhere to their prescribed exercise regimens.
Findings
After testing, I gathered responses to the prototypes for validation or challenging of the goals of the prototype. These are the results of the testing.
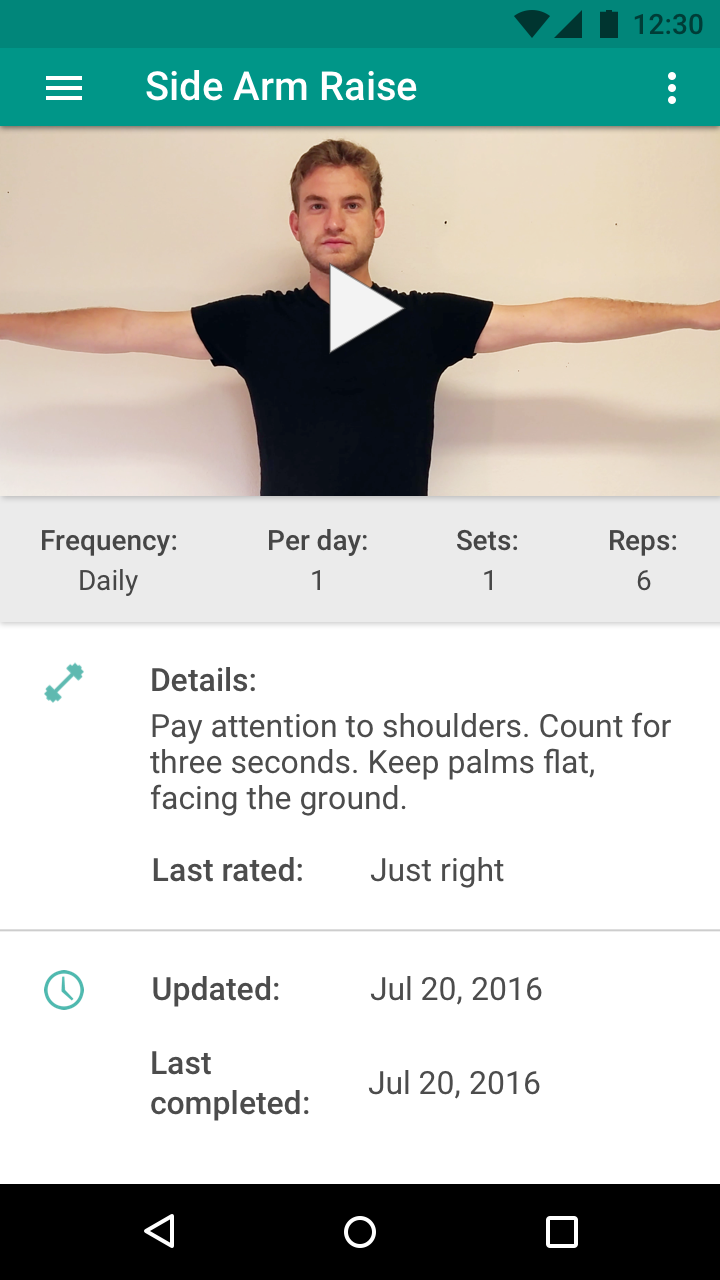
Video Recording
"Confidence ratings increased from pre-video to post-video.
[The video] basically removes all doubt."
— Participant 2
Real Time Feedback
"We didn’t have a representation of the patient on the screen while they were completing their exercises. Participants were unsure if they were completing their exercise correctly, while playing the game.
I still don’t know if I’m doing it correctly in real time."
— Participant 1
Game Distraction
"The games that we let participants play were, on occasion, too engaging or distracting.
I completely forgot to focus on my shoulder blades because I was completely distracted by wondering what I was going to see next."
— Participant 1
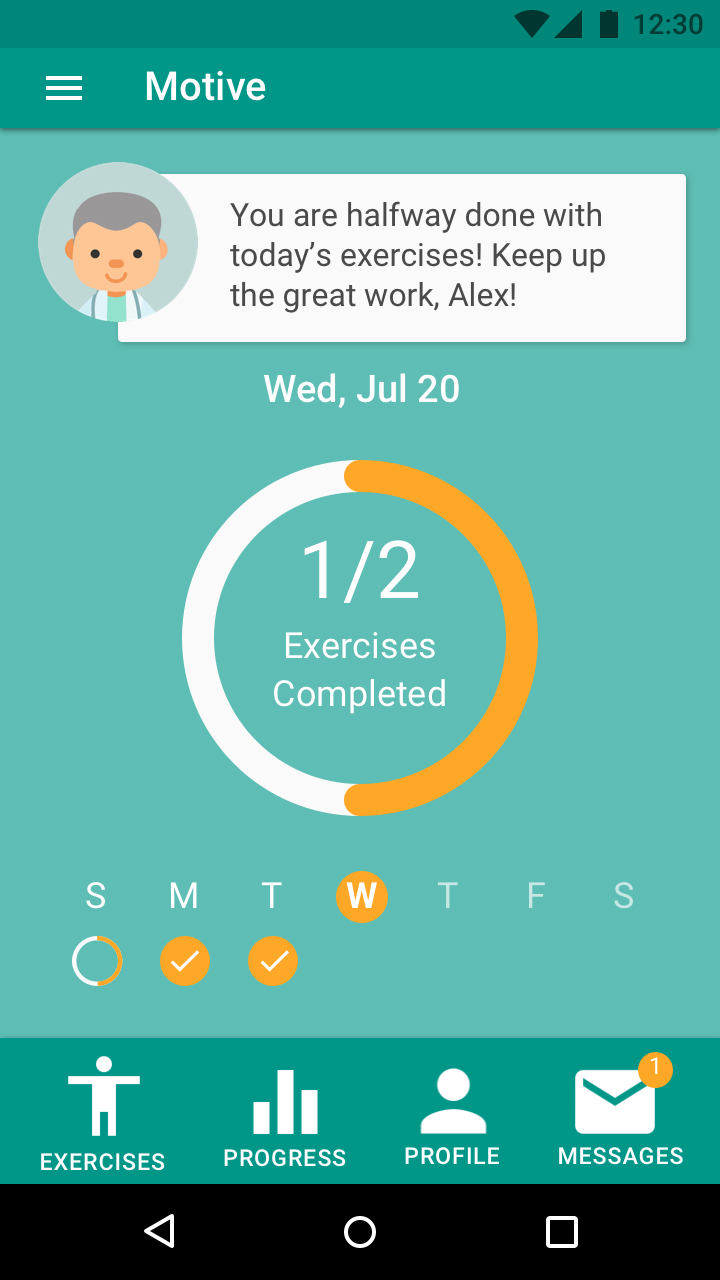
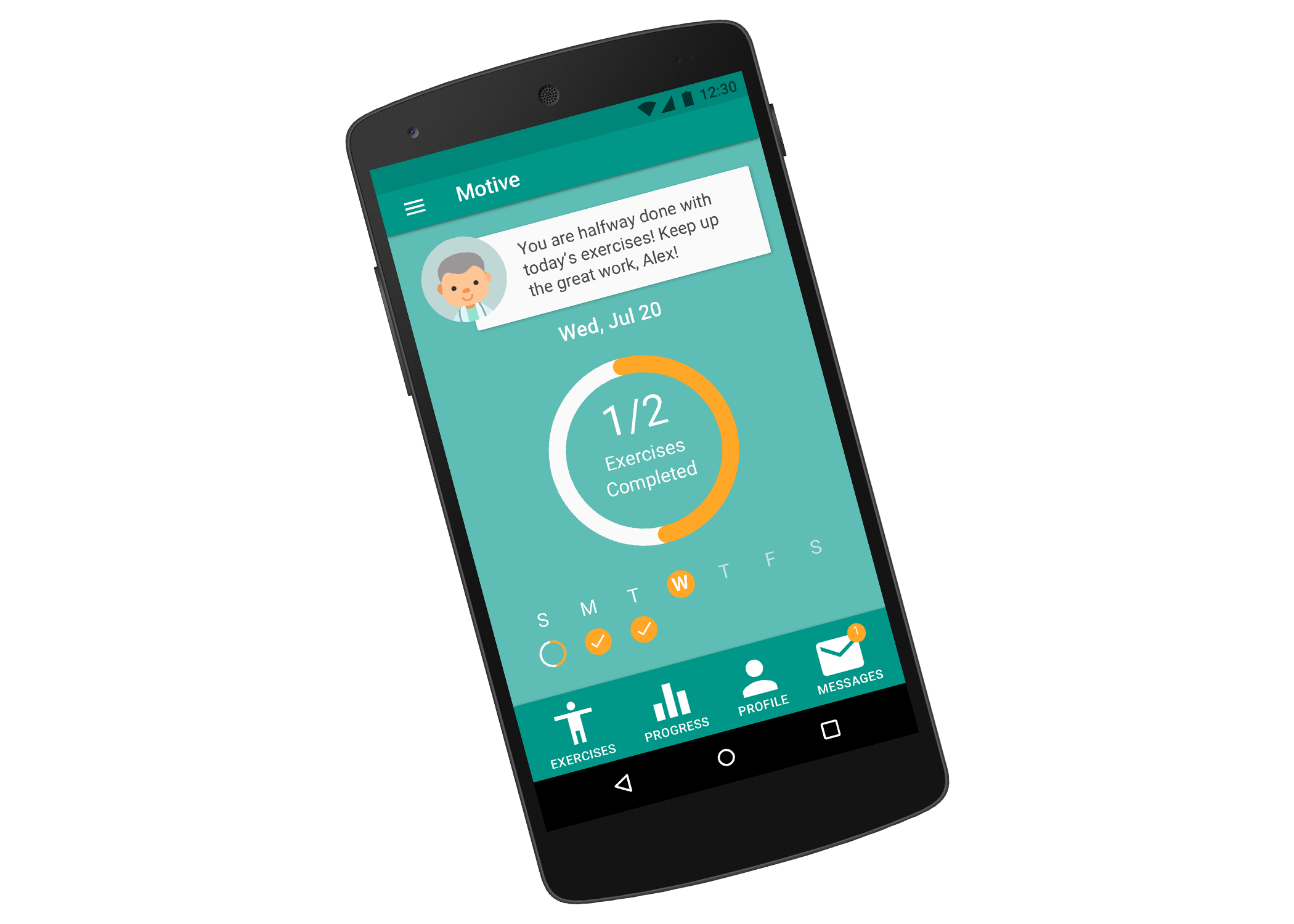
Companion App
"Participants reported that they found the mobile companion application very useful, even without the Kinect.
I could imagine the app being a great option for when I’m traveling and don’t have a Kinect on hand."
— Participant 2
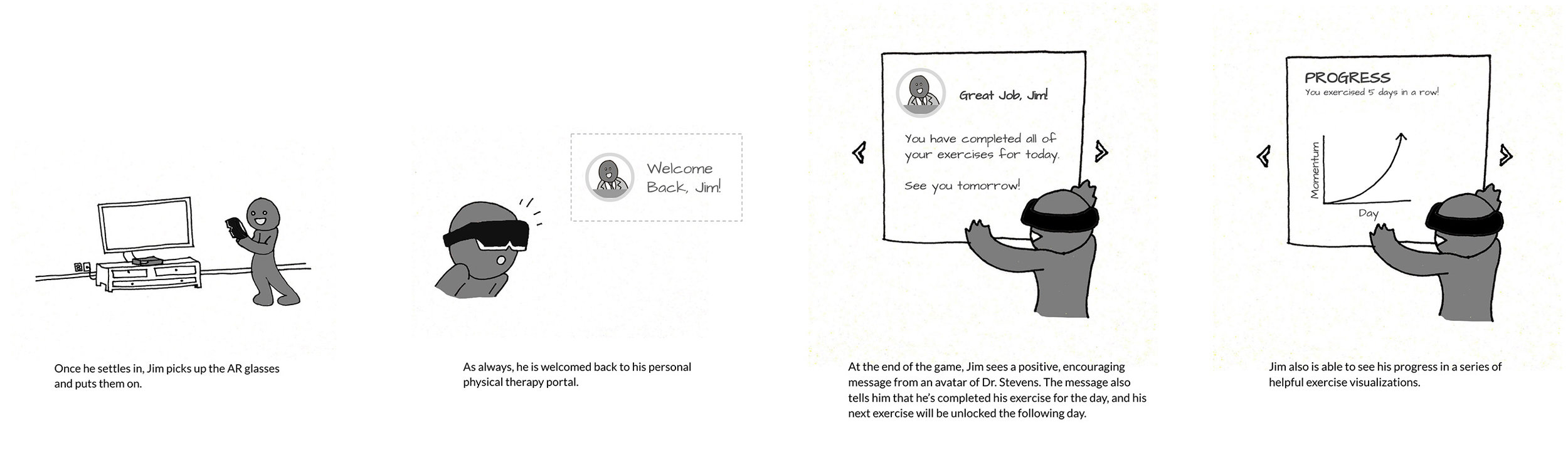
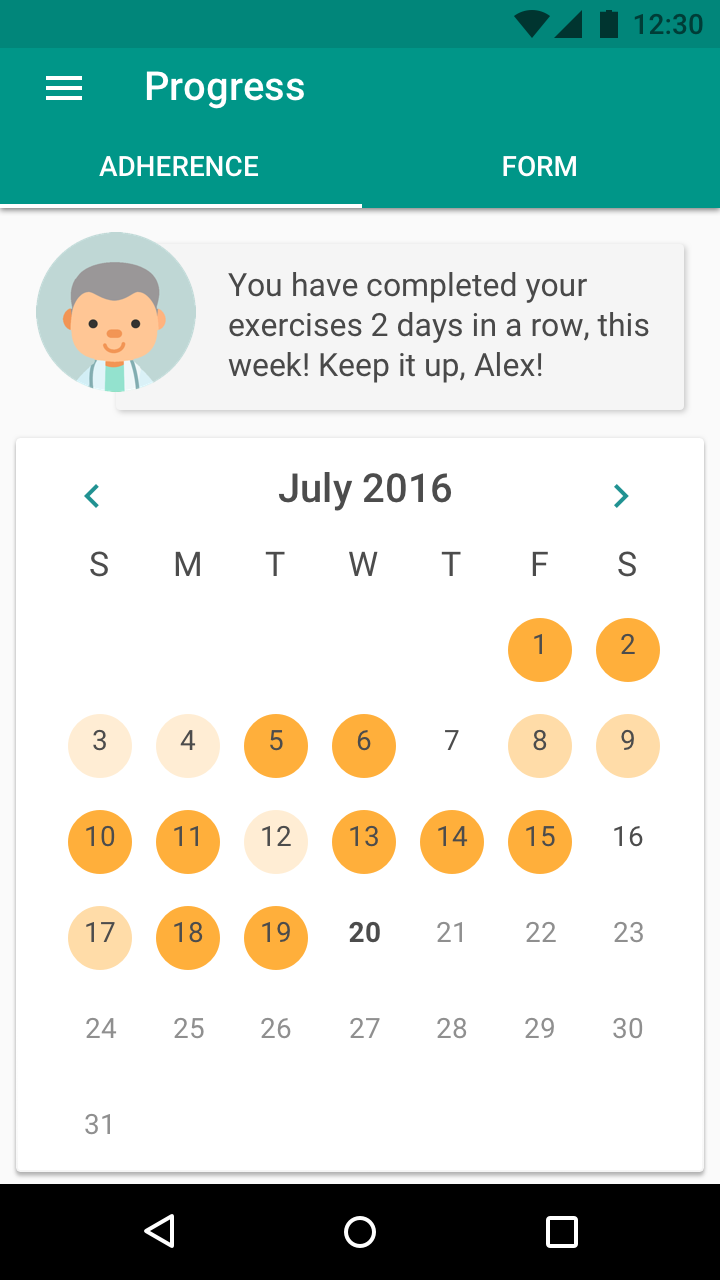
Progress Visualization
"Patients reported the visualizations making their progress more clear and being more confident in their recovery.
It’s in a visual form, so [the progress visualization] tells me I’m making progress even if I don’t know if I am."
— Participant 2
Production
The final design is a physical therapy assistant that motivates patients to complete their home exercises through reference videos, exercise reminders, engaging gameplay and progress reports.
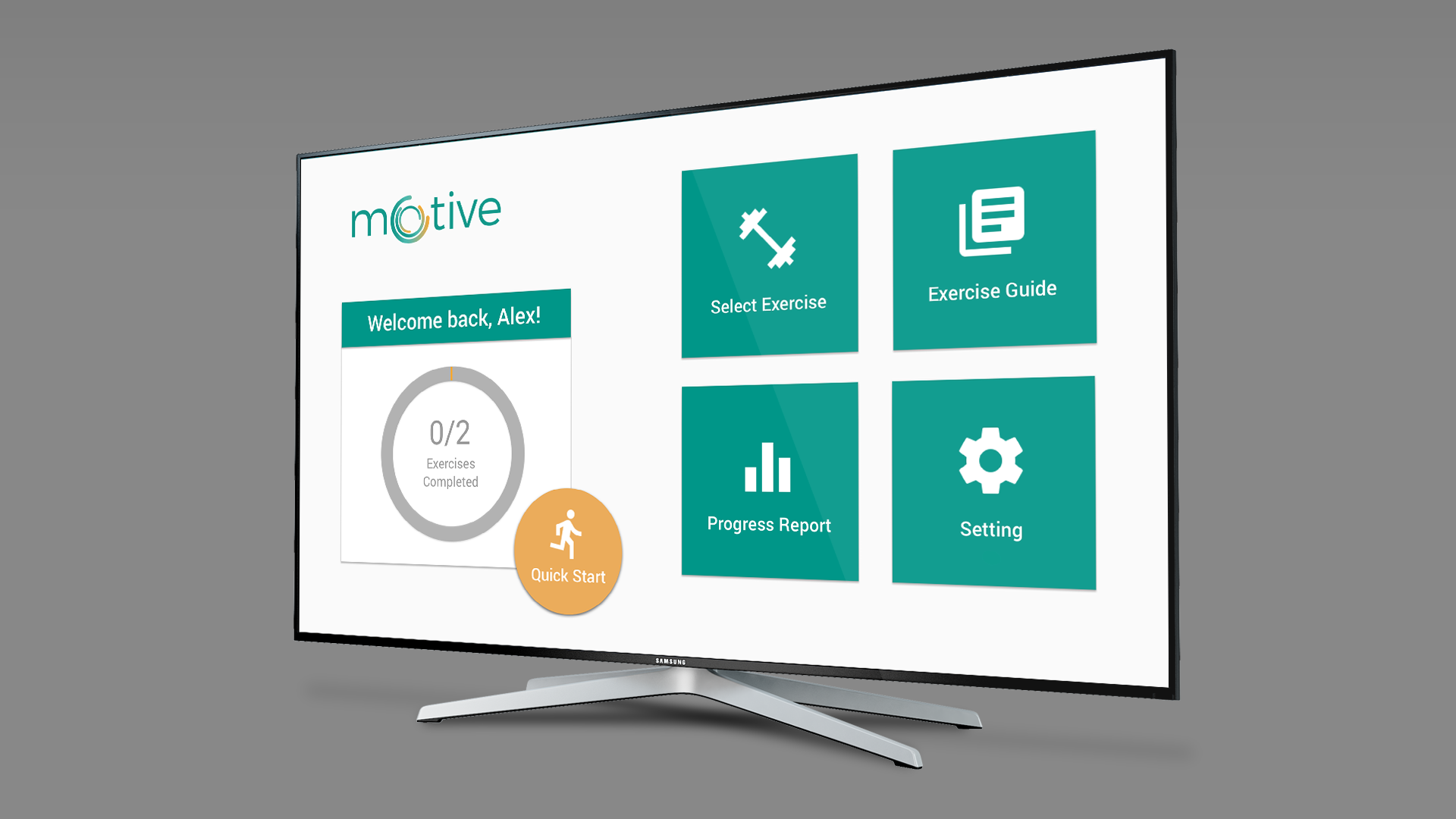
Kinect System
The mobile data is then synced to a motion tracking device in the patient’s home. Here, motion based exercise games are generated to break up the monotony of physical therapy. Progress reports likewise reassure patients that they are on the path to recovery.
Final Word
Ultimately, Motive succeeded in adding value to the physical therapy experience by empowering patients to take ownership of their recovery, providing confidence building reference materials, visualizing progress and breaking up the monotony of physical therapy -- as confirmed by experts and physical therapy patients. Unlike existing products, Motive accomplishes all of these objectives without requiring additional work on the part of physical therapists.